Contact us
Our team would love to hear from you.
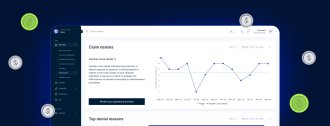
This page explains how medical claims management tools work, what to expect from them, and how to reduce denial-driven revenue leakage across the claims lifecycle.
When the claims process is fragmented across billing software, practice management systems, manual spreadsheets, and disconnected payer portals, organizations pay for it in three ways: time, cash flow, and compliance exposure.
Custom medical claims software enables healthcare providers to:
Medical claims management software automates and optimizes the full process of claims handling, providing benefits to all parties:
A healthcare provider collects patient information, services provided, and diagnosis/procedure codes.
The healthcare provider submits the claim either to a clearinghouse, which forwards it to the insurance payer after validation, or directly to the insurance company.
After receiving the claim, the payer evaluates the validity of the claim based on specific insurance policies.
If the claim is accepted, the payer settles the amount to be paid by the claimant based on the patient’s health insurance plan and reimburses the remaining amount to the healthcare provider.
The payer then sends the EOB statement to the patient, outlining the services provided and payments covered by both parties. The claim is officially closed.
If the payer has denied the claim because of missing data, invalid medical codes, or other problems, the healthcare company can rectify the errors and resubmit the claim.

“Claims information differs from payer to payer, which has caused healthcare providers a lot of trouble. Having a solution that collects, standardizes, and visualizes all valuable information paves the way for smart and data-driven decisions.”
Healthcare Solutions Consultant
Both ready-made and custom claims management tools come equipped with multiple functionalities. The most popular features of bespoke medical claims software include:
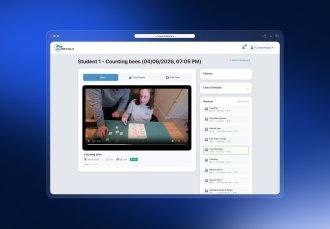
We developed a management system for enhanced medical billing and insurance claim submission and processing.
Healthcare organizations are constantly facing challenges that impact both revenue cycle efficiency and financial performance. Among the key obstacles are:
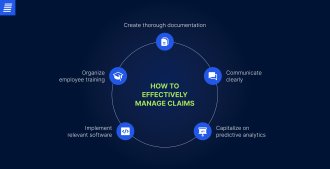
To manage medical claims with maximum efficiency and achieve financial visibility, healthcare organizations follow the principles desribed below.
By combining ML algorithms, statistical models, and historical and current data, predictive analytics helps healthcare providers flag fraudulent claims early, improve claims accuracy, and reduce claims processing time.
Maintaining an accurate and safeguarded record of all medical claims—confidential patient information, diagnosis codes, and treatment details—ensures timely and accurate claims submission, reduces the risk of denials, and provides transparency in the organization’s financial performance.
Transparent communication inspires trust in patients. To establish an effective connection, keep patients informed about the claims processing steps, use patient engagement tools, provide timely updates on claims status, and follow legal communication guidelines.
If you want to eliminate mistakes in claims processing, avoid claims rejections and denials, and minimize reimbursement delays, implement health insurance claims management software. With features like claims intake, data analytics, and reporting, medical claims processing systems address each step of the claims lifecycle, flag fraudulent claims early, streamline documentation, and ensure timely updates to both patients and providers.
Training sessions help employees explore software features like claims submission, coding compliance, and rejection and denial management to work with billing software more efficiently and securely.

A web-based application designed to streamline customer claims processing for a company working in geographically dispersed markets.
Our goal is not just automating tasks and streamlining workflows; we aim to uncover where revenue leaks, where claim denials originate, and where manual processes create risk to your financial stability, data security, and long-term claims performance. We then design our medical claims management software services around these vulnerabilities, turning them into opportunities to maximize revenue across your health systems.
Custom medical claims management solutions connect clinicians, claimants, and insurance payers in a single, controlled system. The result: fewer administrative burden, patient satisfaction, and financial stability for all parties involved.
If your current claims workflow is driving rework, delays, and revenue leakage, contact us to address this with a compliant, scalable technology solution.

Medical claims management is the structured process that begins with creating and submitting claims to an insurance company and continues through adjudication, payment, or resubmission if corrections are required.
Modern claims processing software supports this workflow and ensures seamless integration with existing healthcare systems.
The main challenges in healthcare claims processing include fraud, compliance issues, data management, security, and inflated patient expectations. To easily overcome these hurdles, use EffectiveSoft’s custom medical claims management software services.
EffectiveSoft brings 21+ years of healthcare IT experience and a delivery approach built for regulated environments. We know what challenges health systems face and design medical claims management software development processes to address them. Other reasons companies choose us include our commitment to quality, focus on compliance and security, use of advanced tools and technologies, unique approach to each client and their pain points, and empathy.
The cost of developing a medical claims management tool depends on the overall complexity of the end product, features incorporated, customization levels, integration capabilities, and other factors. If you need an exact quote for your project, contact our team.
Yes, medical claims management software solutions can integrate with EHRs/EMRs, practice management systems (PMSs), medical billing software, insurance clearinghouse tools, and other healthcare IT solutions.
Medical claims software improves reimbursement rates by catching errors and payer-rule mismatches before claims leave your medical billing software. It also standardizes claim data, reduces coding and documentation gaps, and speeds up denial follow-up with clear status tracking and faster resubmissions. The result: faster claims management, fewer avoidable denials, shorter reimbursement cycles, and more revenue.
Yes, AI in healthcare claims processing can significantly improve speed, accuracy, and reimbursement outcomes. AI models analyze large volumes of historical data about to detect patterns behind denials, flag missing documentation, and identify coding inconsistencies before submitting claims. ML algorithms can predict the likelihood of rejection, helping teams prioritize high-risk claims. Natural language processing (NLP) extracts relevant data from clinical notes and unstructured documents, reducing manual entry and errors. AI also strengthens fraud detection by identifying anomalies in billing behavior and claim patterns in real time.
The implementation of medical claims software typically takes 3 to 6 months. This includes workflow analysis, architecture design, development, integration, testing, and staff training. For enterprise-grade software with advanced analytics, complex payer rules, and multiple integrations, the timeline can extend to 12 months.
The biggest variables are data quality, the number of third-party integrations, and how fragmented current claims workflows are. A clear discovery phase shortens delivery time and reduces rework later.
Can’t find the answer you are looking for?
Contact us and we will get in touch with you shortly.
Our team would love to hear from you.
Fill out the form, and we’ve got you covered.
What happens next?
San Diego, California
4445 Eastgate Mall, Suite 200
92121, 1-800-288-9659
San Francisco, California
50 California St #1500
94111, 1-800-288-9659
Pittsburgh, Pennsylvania
One Oxford Centre, 500 Grant St Suite 2900
15219, 1-800-288-9659
Durham, North Carolina
RTP Meridian, 2530 Meridian Pkwy Suite 300
27713, 1-800-288-9659
San Jose, Costa Rica
C. 118B, Trejos Montealegre
10203, 1-800-288-9659